A Guide to Clinical Differential Diagnosis of Oral Mucosal Lesions
Course Number: 110
Course Contents
Autoimmune Diseases
Autoimmune diseases are characterized by blisters and painful ulcers of slow onset. The lesions may get better and worse, but they are persistent and chronic. Lesions do not heal in a predictable period of time. Lymphadenopathy is typically not present.
Pemphigus vulgaris* is a painful autoimmune disease in which the patient forms antibodies to a component of desmosomes located in the stratified squamous epithelium. This results in loss of adherence of epithelial cells and the formation of intraepithelial blisters. The blisters are fragile and quickly rupture forming painful ulcers or erosions which heal slowly. Large areas of skin and mucosa can be involved and may cause serious problems with infection. A Nikolsky sign may be present. Oral lesions eventually form in almost all patients and may be the initial site of lesions. Pemphigus usually begins in mid to late adult life.
Management of pemphigus vulgaris involves an incisional biopsy to establish a definite microscopic diagnosis. Immunofluorescence studies of biopsy material are necessary to make a definitive diagnosis of pemphigus. The disease is treated aggressively with corticosteroids or other immunosuppressive drugs. Without treatment the disease can be fatal. With aggressive treatment, the disease can often be managed successfully, but may still be fatal due to complications associated with the medications.
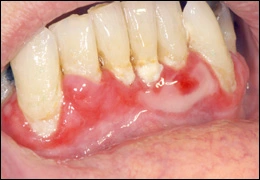
In mucous membrane pemphigoid (cicatricial pemphigoid)* antibodies are directed against antigens in the basement membrane. This causes a separation between the surface epithelium and the underlying connective tissue, resulting in a subepithelial blister. Mucous membrane pemphigoid involves primarily oral mucosa, but mucosa of the nose, pharynx and vagina may also be involved, as well as the skin. A Nikolsky sign may be present. Mucosal and skin blisters rupture to form painful ulcers. Involvement of the gingiva can lead to sloughing of the epithelium, sometimes called desquamative gingivitis.
Mucous membrane pemphigoid
Desquamative gingivitis can also be present in lichen planus and pemphigus. Mucous membrane pemphigoid is also known as cicatricial pemphigoid because the ulcers can cause scarring of the mucosa and conjunctiva leading to blindness. It is most common in middle-aged and older adults.
Without treatment it usually requires weeks to months for the ulcers to heal. Mucous membrane pemphigoid may appear clinically similar to pemphigus vulgaris and erosive lichen planus. An incisional biopsy with immunofluorescence studies is important to establish a definitive diagnosis. Mucous membrane pemphigoid cannot be cured, but topical and systemic corticosteroids, as well as other medications, are used to control the disease. The disease has exacerbations and remissions, with or without treatment.
Bullous pemphigoid is a chronic autoimmune disease that involves the skin and, less commonly, the mucosa. The autoimmune reaction is directed against antigens in the basement membrane resulting in separation between the surface epithelium and the underlying connective tissue. Lesions consist of vesicles and bullae that rupture to form painful ulcers. Oral lesions in bullous pemphigoid resemble those of mucous membrane pemphigoid. Bullous pemphigoid does not cause scarring and tends not to be as chronic as mucous membrane pemphigoid. Bullous pemphigoid is managed with systemic corticosteroid medications. The prognosis is good.
To view the Decision Tree for Oral Mucosal Lesions, click on one of the options shown.
To view the Decision Tree for Oral Mucosal Lesions, click on one of the options shown.


 View Interactive
View Interactive View as PDF
View as PDF View as GIF
View as GIF