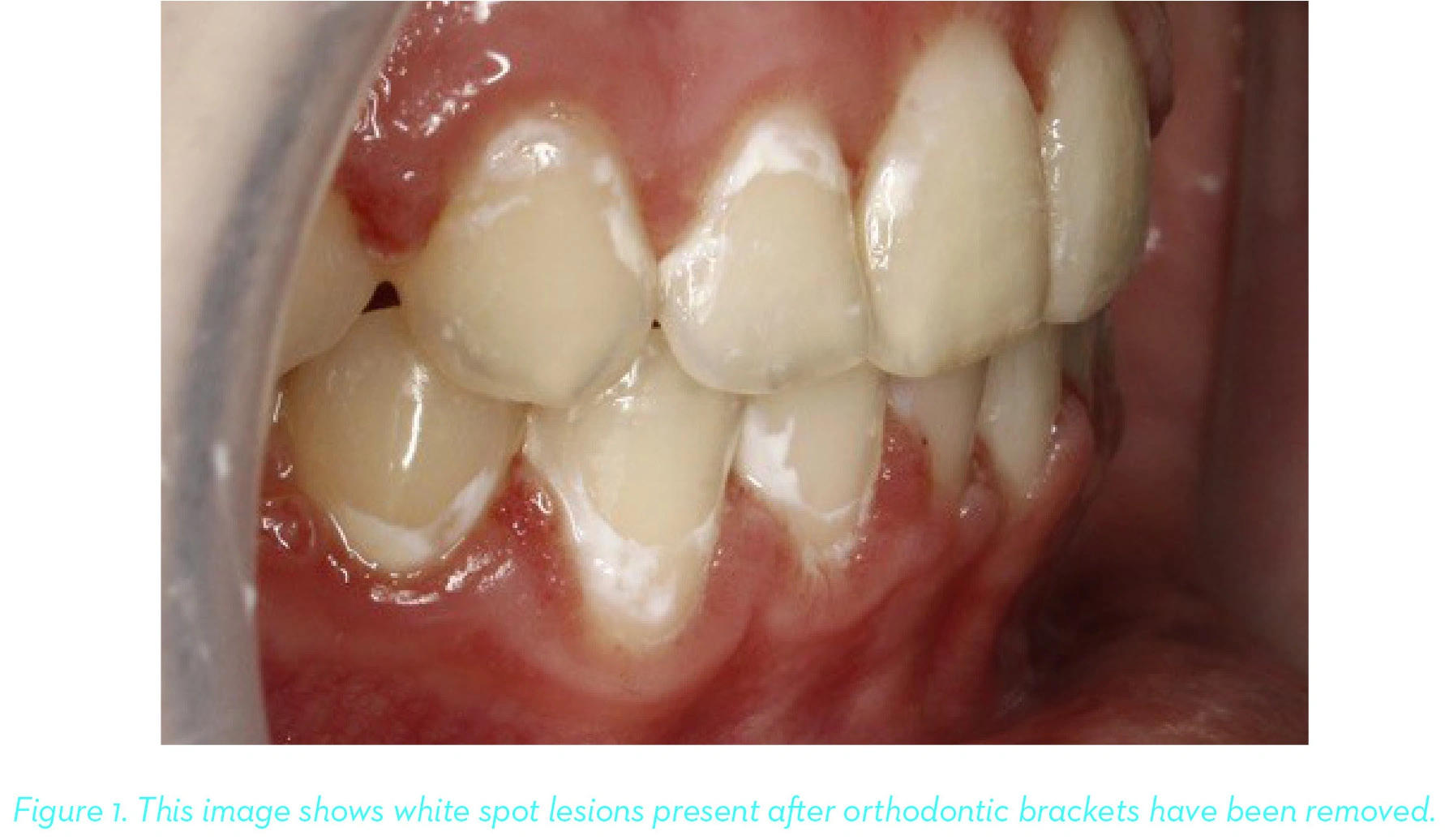
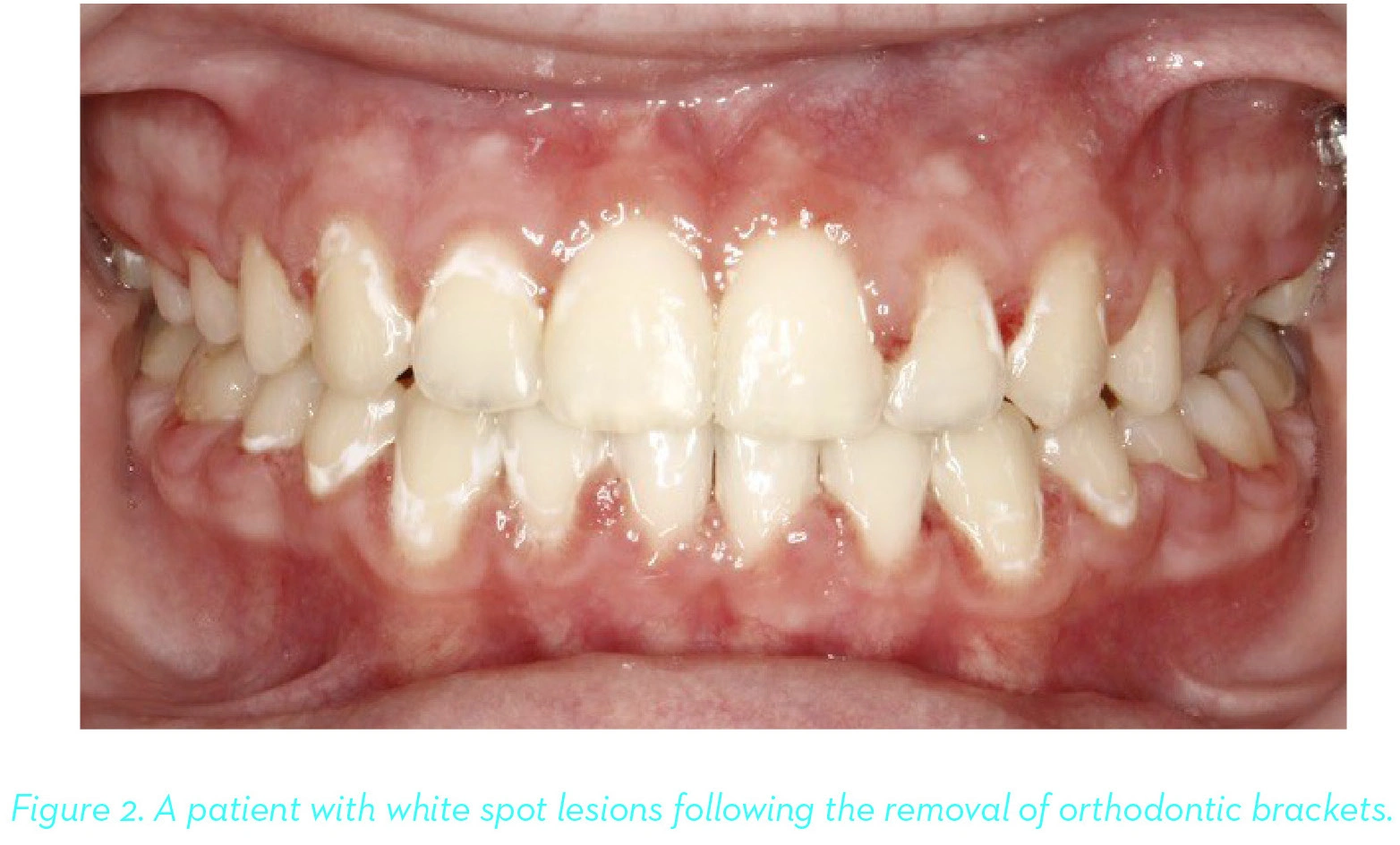
White Spot Lesions
White spot lesions (WSLs) are serious side effects of orthodontic therapy and can eventually lead to the development of caries. In fact, WSLs are considered one of the most common adverse effects of orthodontic treatment and the increase in incidence of WSLs exposes the orthodontist and general dentists to the risk of malpractice and litigation.
These lesions occur as a result of demineralization caused by plaque accumulations around brackets and aligners. This common problem can be serious with long-lasting esthetic consequences and may require expensive and invasive future restorative treatment.
The challenge facing practitioners
Fixed multi-bracket orthodontic treatment creates an environment wherein bacterial plaque accumulates on enamel surrounding brackets. This plaque is difficult to remove mechanically, plus, the patients often exhibit poor oral hygiene and a lack of follow-up prophylaxis. As pH in the plaque drops, the acid-accelerated demineralization of the enamel surface occurs, leaving a white porous surface that is susceptible to future progression to caries.
Various treatments for WSLs have been utilized but none have been universally successful. The basic problem is that once demineralization of the enamel begins, it is very difficult to stop or control.
The commonly used treatments involve the use of topical fluorides, including toothpastes, mouth washes and fluoride varnishes. Other remineralizing agents such as casein phosphopeptide-amorphous calcium phosphate (CPP-ACP) have also become popular.
However, while all agents offered a degree of protection, there is no consensus regarding the actual success of these treatments.†
Professional application of fluoride varnishes is helpful, but success depends on excellent patient compliance with dietary and home health care procedures (toothbrushing), which is often lacking among these patients.
Protection is key
As noted above, once white spot lesions occur there are no universally acceptable treatments. To control this problem a specific treatment philosophy is needed:
Phase I: Begin protection before demineralization occurs, as once lesions occur, they are difficult to control.
First, one should insist that patients have:
A prophylaxis and comprehensive oral hygiene instruction before treatment
Continue to have regular prophylaxes during treatment
Oral hygiene status continuously monitored by the orthodontic office
Secondly, parents and patients must be counselled on the importance of reducing dietary sugars and acids to help reduce the pH of the plaque to the enamel surfaces. Reducing the intake of acidic beverages such as sodas, sports and energy drinks and flavoured bottled water is mandatory.
Also, patients should be aware that “how they drink their drinks” is critical to decrease the acid contact to their teeth. They should be quickly swallowed and not “swished” or held in the mouth. Sugary, sticky foods should also be avoided.
Thirdly, practitioners should insist that patients use an oscillating-rotating electric toothbrush, as this is the most efficient tool for removing plaque deposits around brackets and aligners. This will also help to reduce gingival inflammation around orthodontic bands, wires, and brackets.2
Finally, the most important source of protection before, during and after treatment is the use of a stabilized stannous fluoride toothpaste.3
Historically, dentifrices containing sodium fluoride have been very beneficial in the worldwide reduction of dental caries. However, with the research and development of stabilized stannous fluoride toothpastes, many additional therapeutic benefits are available.
These include bacteriostatic (reduce acid production) and bactericidal (kill bacteria) properties of the stannous ion for gingival health and, importantly, the deposition of an insoluble layer of stannous oxide and stannous fluorophosphate on the enamel surface, which creates a physical barrier to acid challenges, hence protection against erosive tooth wear. Additionally, this stannous barrier also forms a smear layer over exposed dentinal tubules and helps to reduce erosive tooth wear and reduce hypersensitivity.2
Phase II: In-Office treatments can help slow developing demineralized lesions
Numerous interventions have been tried, including the use of sodium fluoride mouthwashes and fluoride varnishes and various remineralizing agents such as CPP-ACP pastes and creams, with varying degrees of success. Fluoride-containing sealants have also been useful and can easily be applied during recall visits. However, it should be emphasized, that while all of the treatments noted above may be helpful, once the WSLs have developed, they are irreversible. Undergoing restorative treatment can be costly to the patient, takes up more practice time, and overall impacts the patient experience and end result. We want our patients to have a successful treatment journey with us and we can achieve this by addressing our patients’ behaviour and preventing demineralized lesions from forming before they start.
Phase III: After appliance removal more invasive restorative procedures are often needed.
Composite resins can be used to hide surfaces with minimal demineralization. Where lesions have progressed to caries, the use of conventional bonded composite materials may be necessary. In severe cases, porcelain veneers or crowns may be needed.
Summary
White spot lesions are an acid-accelerated problem. To help manage this significant complication to orthodontic therapy, patients must reduce intake of dietary sugars and acids to help minimize demineralization of enamel. Patients, whom a change of dietary habit may prove too difficult: recommend a change of tools, to an oscillation-rotation powerbrush. Only stannous fluoride or stannous chloride have the potential for slowing the progression of erosive tooth ware (ETW).7 It is incumbent upon us to exhaust every opportunity for the prevention of irreversible demineralization in our patients. By institutionalizing a proactive approach in our protocols and striving for excellent oral hygiene in our patients, executing frequent prophylaxis, and recommending the use of a stabilized stannous fluoride toothpaste, we will help our patients achieve a predictable, happy, healthy smile.
Ward Noble, DDS, MS, MSEd, graduated from UCSF and completed a specialty program in prosthodontics at University of Michigan. He served as a faculty member at UCSF from 1970-2005. After 35 years in private practice, he became a professor in the Department of Preventive and Restorative Dentistry at the Dugoni School of Dentistry, where he has received teaching awards from both students and faculty. He has given more than 250 presentations both nationally and internationally and has written numerous articles as well as chapters for dental textbooks. He mentors the multidisciplinary seminars with the orthodontic residents and faculty at the University of Pacific.
References:
1. Khoroushi M and Kachule M. Prevention and treatment of white spot lesions in orthodontic therapy. Contemp Clin Dent 2017 Jan-Mar;8(1):11-19. PMID: 28566845.
2. West NX, He T, Zou Y, et al. Bioavailable gluconate chelated stannous fluoride toothpaste meta-analysis: Effects on dentine hypersensitivity and enamel erosion. J Dent. 2021 Feb; PMID: 33383100.
3. Biesbrock A, He T, et al. The effects of bioavailable gluconate chelated stannous fluoride stannous fluoride dentifrice on gingival bleeding: Meta-Analysis of eighteen randomized controlled studies. J Clin Periodontol 2019 Dec;46(12):1205-1216. PMID: 31562774.
4. Grender J, Adam R, Zou Y. The effects of oscillating-rotating electric toothbrushes on plaque and gingival health: A meta-analysis. Am J Dent. 2020;33(1):3-11.
5. West NX, He T, Zou Y, DiGennaro J, Biesbrock A, Davies M. Bioavailable gluconate chelated stannous fluoride toothpaste meta-analyses: Effects on dentine hypersensitivity and enamel erosion. J Dent. 2021 Feb;105:103566. doi: 10.1016/j.jdent.2020.103566. Epub 2020 Dec 28. PMID: 33383100.
6. Biesbrocck A, et al. The effects of bioavailability gluconate chelated stannous fluoride dentifrice on gingival bleeding: Meta-Analysis of eighteen randomized controlled trials. Journal of Clinical Periodontology; December 2019.
7. Carvalho TS, Colon P, Ganss C, Huysmans MC, Lussi A, Schlueter N, Schmalz G, Shellis RP, Tveit AB, Wiegand A. Consensus report of the European Federation of Conservative Dentistry: erosive tooth wear--diagnosis and management. Clin Oral Investig. 2015 Sep;19(7):1557-61. doi: 10.1007/s00784-015-1511-7. Epub 2015 Jul 1. PMID: 26121968.